Hydrocele Sclerotherapy Treatment
- No hospital
- No surgery
- No sutures
- No scars
- Outpatient
- Image guided
- Fast recovery
- Targetted therapy
- Low risk
- Successful
- Proven benefit
- Quick
Setup an appointment
Why treat a scrotal hydrocele?
A hydrocele is a collection of fluid in the scrotum that causes swelling, which is soft and often painless. The swelling however may be unsightly and uncomfortable during intercourse or physical activity. A hydrocele is diagnosed by ultrasound, which can be done in the office.
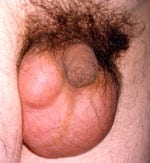
Am I a candidate for hydrocele sclerotherapy?

If the hydrocele becomes too large or causes a level of discomfort then treatment maybe recommended. The first step is a diagnosis, which can be done by an ultrasound in the office. Our doctor is a board certified imaging specialist in addition to specializing in minimally invasive procedures and will perform the diagnostic ultrasound during your visit if you have not had one. If you have already had an ultrasound, generally the first step is to have a consultation to understand the procedure, preparation and expected results. Occasionally, the consultation and treatment can be done at the same time.
Treatment Options
There are two types of treatments for hydroceles: surgery and sclerotherapy.
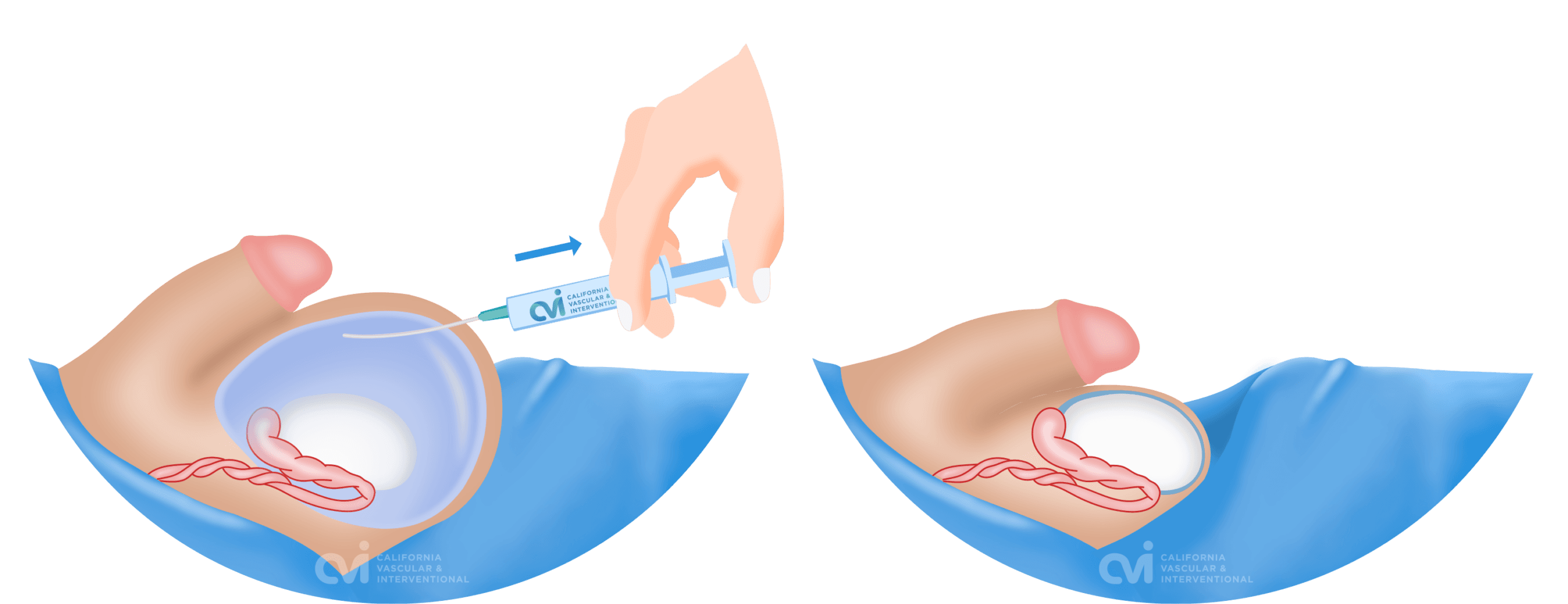
Hydrocele Aspiration & Sclerotherapy
Sclerotherapy was first reported in 1975 as a treatment alternative for hydroceles with no downtime.5 Sclerotherapy is an outpatient procedure performed in the office that involves removing the fluid collection through a small tube followed by injection of a medication (sclerotherapy) that helps close the cavity containing the fluid. Our specialist applies a local anesthetic to make the procedure essentially pain-free. There is no anesthesia required and any discomfort is typically treated with anti-inflammatory medication, such as Ibuprofen. There is no downtime, stitches or incisions. You will walk out of the office after the procedure.
This is a minimally invasive, quick, safe, and effective treatment for a hydrocele. The risk of complications is low and patient satisfaction is high. Unlike surgical excision, you will not need narcotics, athletic scrotal support, ice or sutures.
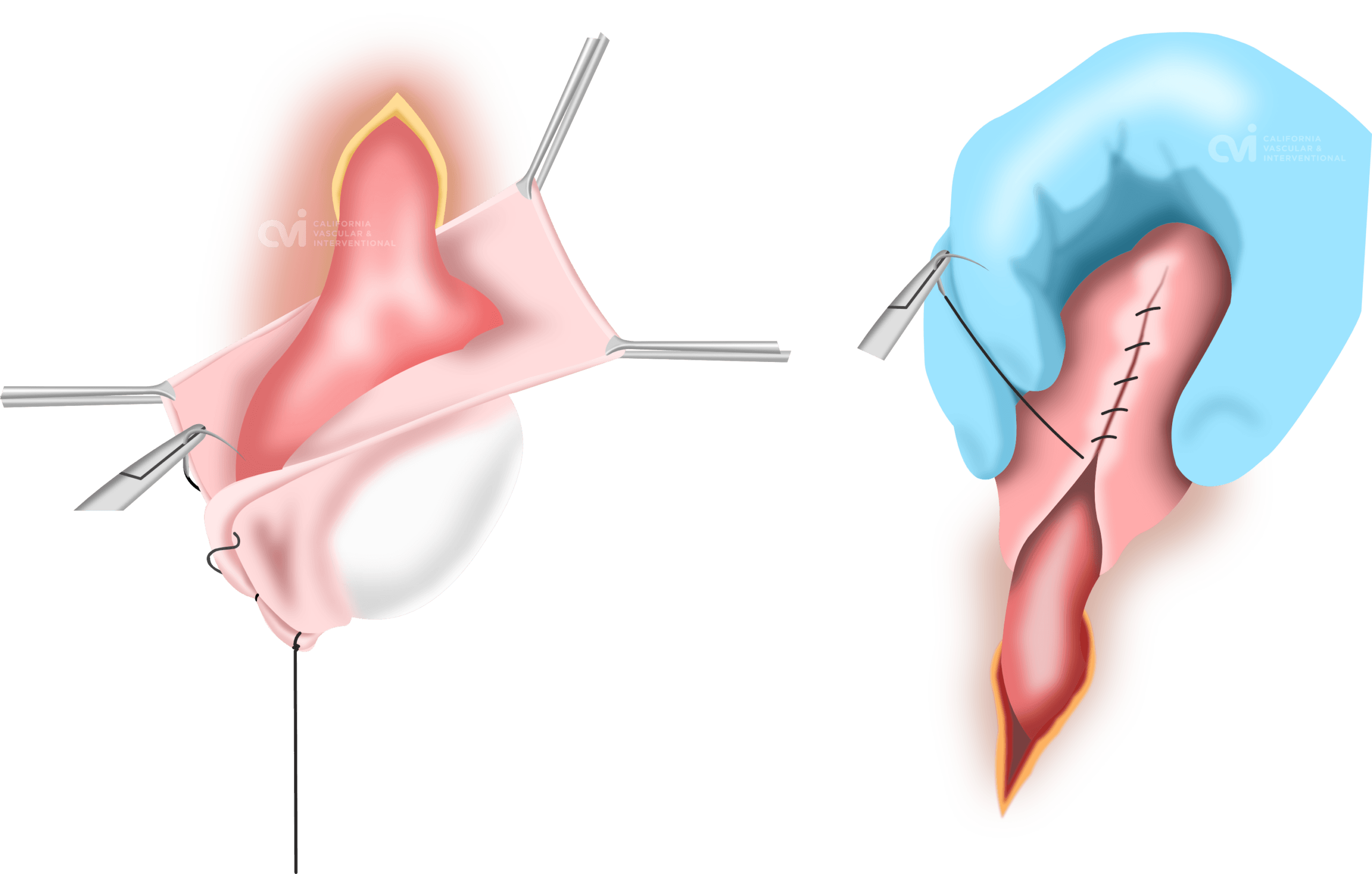
Surgical Hydrocelectomy
While we don’t perform surgery you should understand and be informed of the surgical option. Surgery continues to be the most common method of treatment for a symptomatic hydrocele.2 During the surgery, the surgeon will make an incision in your scrotum and drain the fluid from around the testicle. The space will then be sutured together. Recovery from surgery can take up to 5 days and you will be provided medication for pain management. Surgical complications include prolonged pain, recurrence, hematoma, infection and injury to the scrotal contents including the testicle, epididymis and/or vas deferens.3 In one study 40% of the patients undergoing surgical hydrocelectomy experienced postoperative complications including edema, hematoma, infection and cellulitis.4
You can watch how hydrocelectomy surgery is performed via the following LINK: VIEWER’S DISCRETION ADVISED: GRAPHIC VIDEO (Please note we are not affiliated)
What is the right treatment for me?
If you’ve been diagnosed with a scrotal hydrocele it’s important to gain at least a basic understanding of your treatment options.
Every approach to treatment has its pros and cons. Ultimately, the treatment you choose will depend on what your doctor recommends and what feels best to you. Some patients obtain surgery while others prefer a non-surgical option such as sclerotherapy, and only seek surgery if the treatment is not effective for them.
You should seek the expert advice of your urologist and our interventional radiologist to further understand your options and expected outcomes.
Our interventional specialist has performed more hydrocele and spermatocele sclerotherapy treatments than any other practitioner. We are the number one recommended and referred to practice for this treatment. In fact, our specialist also performs sclerotherapy of kidney and liver cysts as well.
Over the years our specialist has developed his own technique based on experience on what works and what doesn’t work. This has increased the success rates while decreasing the discomfort. Other practitioners have limited experience in this treatment and they typically perform hydrocele aspirations blindly by jabbing a needle into the scrotum without ultrasound. One problem with this technique is that it almost always leave some fluid when the procedure is done blindly with a needle and without ultrasound guidance. If there is any residual fluid then the sclerotherapy does not work very well. This is just one of the many details that are important in having a successful outcome.
You can rest assured that your experience will be much more pleasant at CVI as the procedure is performed with precision using ultrasound guidance by our specialist. Our specialist has performed over 5,000 ultrasound guided procedures in addition to his experience in performing sclerotherapy injections.
Can't I just have aspiration to remove the hydrocele fluid?
Aspiration alone will not be sufficient. If your specialist only removes the fluid it will only be a matter of time that the hydrocele will return causing your symptoms again. Sclerotherapy is important as it closes the cavity, preventing the fluid from returning.
Our specialist performs the aspiration first using ultrasound-guidance. The ultrasound shows precisely the location of the needle so that the testicle or adjacent structures do not get punctured, essentially eliminating any risk thereof. Make sure that your specialist performing this procedure is trained in ultrasound-guided procedures.
My Urologist tried sclerotherapy and it didn't work. Is this the same?
No.
Most urologist will not offer aspiration and sclerotherapy. For urologists that do, they do not perform the procedure with the same technique as our specialist. There are several reasons why sclerotherapy by your urologist failed. The main reason is the lack of ultrasound guidance. Ultrasound confirms that all of the hydrocele fluid has been removed before injecting the medication. Any fluid left behind will dilute the medication rendering it inactive. Urologist perform this procedure blindly with a needle. There is no way to know if there is any fluid left in this manner. Needle aspiration is also not as effective in removing all of the fluid.
Our specialist performs the aspiration first using ultrasound-guidance. Ultrasound is used throughout the procedure to make sure the procedure is performed adequately and safely. The ultrasound shows precisely the location of the tube so that the testicle and adjacent structures do not get punctured, essentially eliminating any risks. Make sure that your specialist performing this procedure is trained in ultrasound-guided procedures. Our specialist performs more sclerotherapy treatments than any other specialist.
Sclerotherapy Cost
We do not accept insurance for sclerotherapy. Since the cost of the sclerotherapy is not covered by insurance, this is ideal for someone who feels strongly about avoiding surgery as there is an out of pocket cost. Please contact our office for the current charges.
Sclerotherapy is Not New
Sclerotherapy is not new! Sclerotherapy has been performed on fluid collections and cysts for decades! Our doctor performs sclerotherapy on large cysts in the liver, kidney and other structures for over 10 years. In other organs, our doctor leaves a drainage catheter and patients return for weekly sclerotherapy sessions until the cyst is gone. Due to the nature of the scrotum our doctor deploys a different method to achieve the same success without having to leave a catheter in place. Patient go home without a catheter, incision, suture or any bandaging.
Results
Sclerotherapy is a non-surgical treatment for scrotal hydroceles that is safe and effective. There are no stitches, major incisions or downtime. You walk out of the office after the treatment. The success rate of a single hydrocele aspiration and sclerotherapy procedure is 75-84% after one treatment, while avoiding the hospital expense and many other complications of surgery.6,7 Surgical hydrocelectomy by comparison has a similar success rate of 84% in one study.4
Large hydroceles would require multiple treatment sessions and have a higher rate of treatment failure. Hydroceles due to tumor, infection, hernia and certain types of hydroceles would not be appropriate candidates for this treatment.
Appointments are available via an online video telehealth platform or in person at one of the offices in Los Angeles, Orange County or San Diego, depending on the doctor’s availability. Contact Us Today. Why should you choose us? Read here.
References:
- Leung ML, Gooding GA and Williams RD: Highresolution sonography of scrotal contents in asymptomatic subjects. AJR Am J Roentgenol 1984; 143: 161.
- Lord PH: A bloodless operation for the radical cure of idiopathic hydrocele. Br J Surg 1964; 51: 914.
- Swartz MA, Morgan TM and Krieger JN: Complications of scrotal surgery for benign conditions. Urology 2007; 69: 616.
- Beiko DT, Kim D and Morales A: Aspiration and sclerotherapy versus hydrocelectomy for treatment of hydroceles. Urology 2003; 61: 708.
- Moloney GE: Comparison of results of treatment of hydrocele and epididymal cysts by surgery and injection. Br Med J 1975; 3: 478.
- Levine LA and DeWolf WC: Aspiration and tetracycline sclerotherapy of hydroceles. J Urol 1988; 139: 959.
- Francis JJ, Levine LA: Aspiration and sclerotherapy: a nonsurgical treatment option for hydroceles. J Urol. 2013 May;189(5):1725-9. doi: 10.1016/j.juro.2012.11.008. Epub 2012 Nov 6.






