
Virtual remote appointments are available. Contact us for a video telehealth evaluation.

All appointments conducted by our Board Certified doctor and not assistants or non-physician providers.
Pelvic Venous Congestion Syndrome
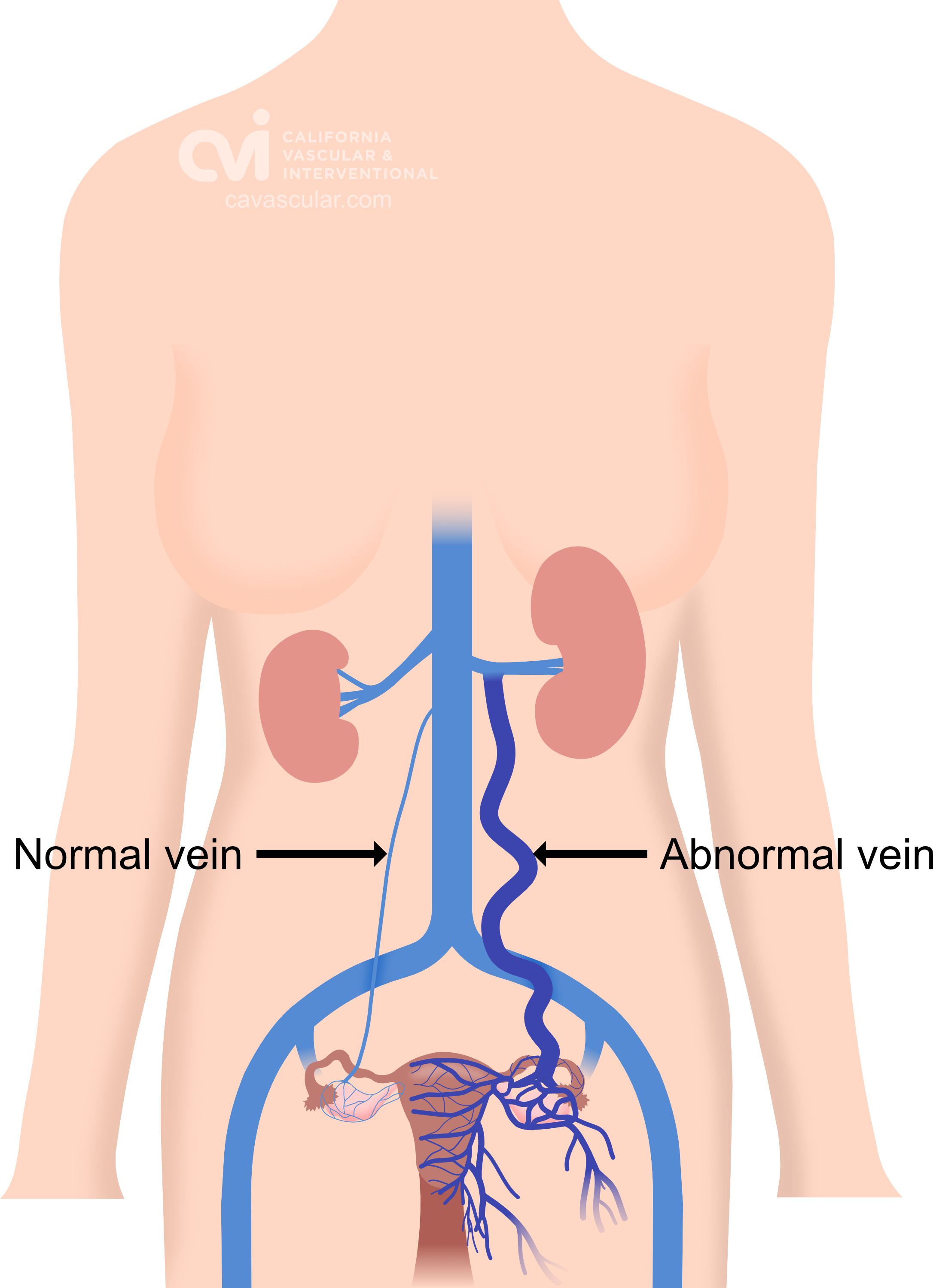 Pelvic Congestion Syndrome (PCS) or Pelvic Venous Congestion Syndrome (PVCS) is essentially varicose veins of the ovaries. Varicose veins are most commonly seen in the legs and are caused by the veins becoming less elastic resulting in abnormal flow of blood causing it to pool in certain areas, leading to enlarged painful veins. This is also what happens to the pelvic veins in pelvic congestion syndrome.
Pelvic Congestion Syndrome (PCS) or Pelvic Venous Congestion Syndrome (PVCS) is essentially varicose veins of the ovaries. Varicose veins are most commonly seen in the legs and are caused by the veins becoming less elastic resulting in abnormal flow of blood causing it to pool in certain areas, leading to enlarged painful veins. This is also what happens to the pelvic veins in pelvic congestion syndrome.
PCS most commonly occurs in young women, and usually in women who have had at least 2-3 children. During pregnancy the ovarian vein can be compressed by womb or increase in size because of the required increased blood flow. This is thought to damage the valves causing them to stop working resulting in abnormal blood flow backwards. This pressure build up causes the pain of PCS and may also cause visible varicose veins around the vulva, vagina, inner thigh, sometimes the buttock and down the leg(s).
The abnormal veins dilate and cause varicose veins around the ovary and uterus because the valves don’t work properly. Blood flow is in the wrong direction, pooling in the veins and causing them to enlarge.
How do you get rid of these? See the next section.
What are the Treatment Options?
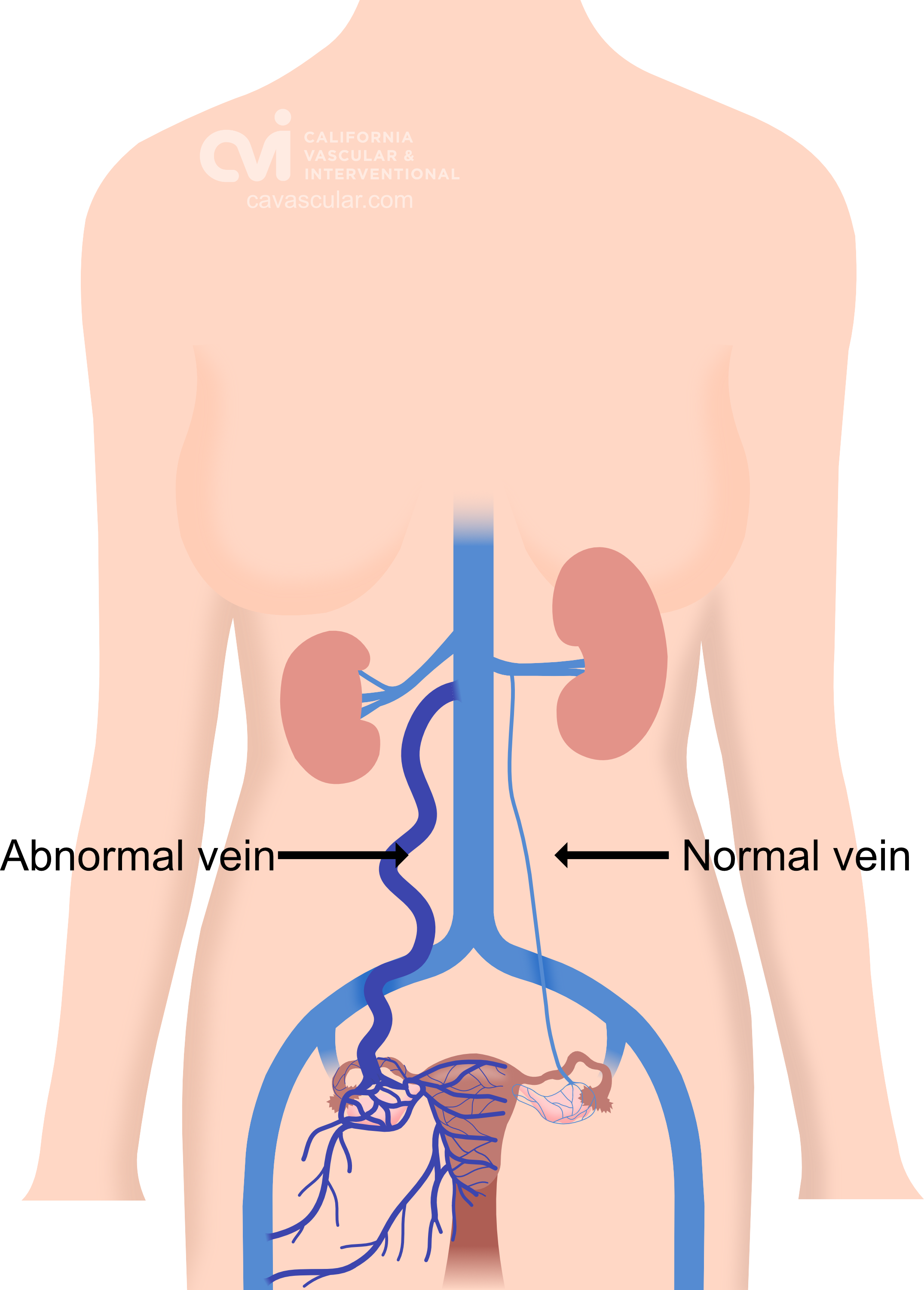 Embolization – The gold standard for treatment is closure of the abnormal veins, similar to varicose veins in the legs. This is called “Ovarian vein embolization." This is an outpatient procedure that requires no sedation or general anesthesia. Read below for further details.
Embolization – The gold standard for treatment is closure of the abnormal veins, similar to varicose veins in the legs. This is called “Ovarian vein embolization." This is an outpatient procedure that requires no sedation or general anesthesia. Read below for further details.
Hysterectomy is sometimes offered however this is not ideal as the abnormal varicose veins are left behind. If there is persistent chronic pain after hysterectomy, ovarian vein embolization is either very difficult or not possible.
Conservative management with hormones is also an option. There are a few medical drug treatments (medroxyprogesterone acetate or more recently, goserelin), which has been shown to be somewhat effective in reducing pain and the size of the varicose veins. This will not however eliminate the abnormal veins and will require continuous medical therapy.
Surgery – Other treatment options are open or laparoscopic surgery to tie the culprit veins. Both these procedures are more invasive than ovarian vein embolization and require a general anesthetic and a longer recovery period. Abnormal veins can also be left behind require repeat surgery or ovarian vein embolization.
What is Ovarian Vein Embolization?
Ovarian vein embolization is a non-surgical outpatient procedure that is performed through a tiny nick in the skin under moderate sedation.
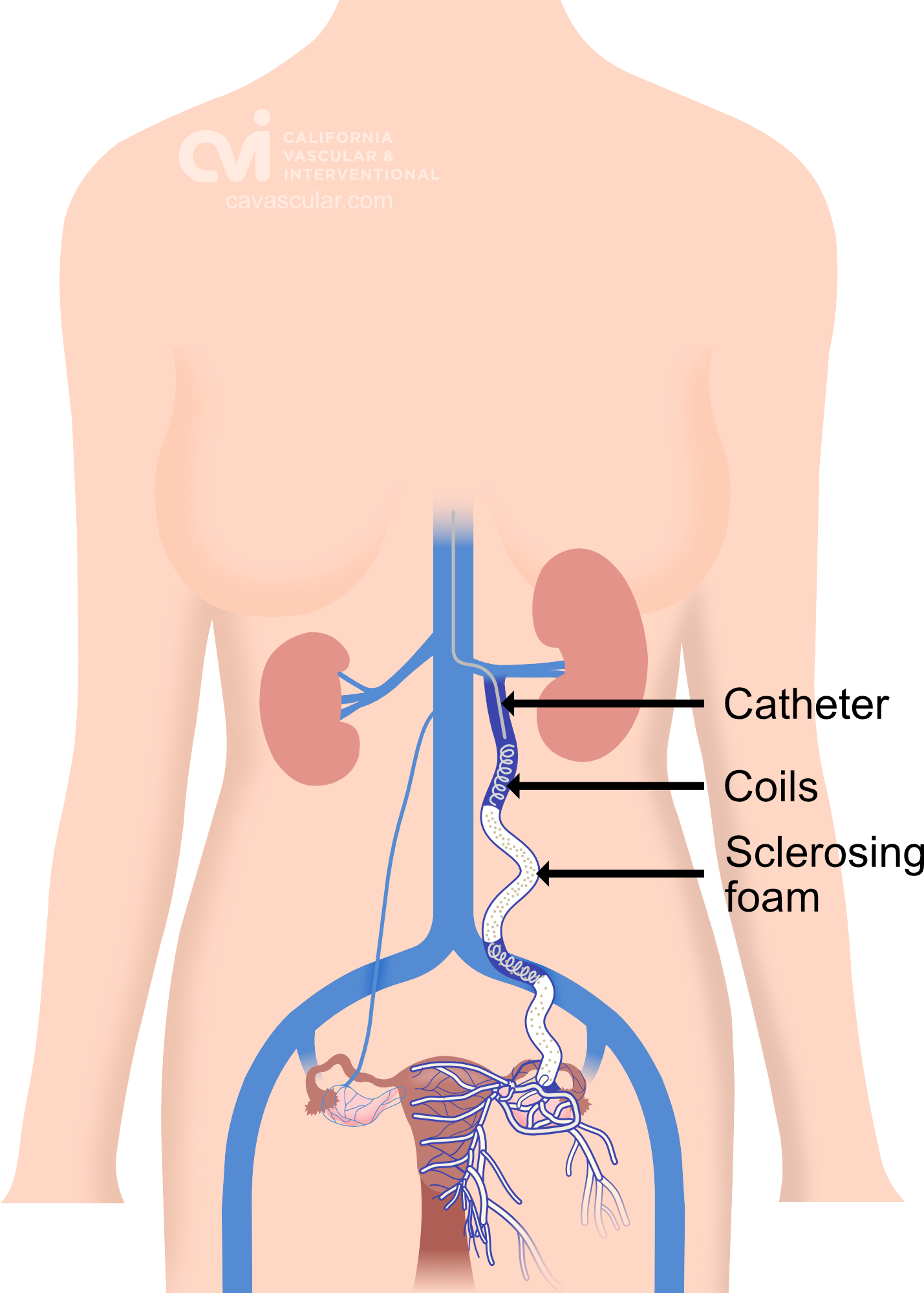
During this procedure, our image-guided specialist will numb the skin and insert a catheter (a tiny tube) into a vein in the neck or groin. The placement is done with precision using ultrasound guidance minimizing pain.
Using x-ray guidance a smaller catheter is then guided into the abnormal ovarian or pelvic veins. The abnormal vein is then treated by placing tiny coils and a specialized fluid causing the vein to seal down. This then restores normal blood flow in the body and improves related symptoms.
There are no stitches, major incisions, hospital stay requirements, or significant downtime. Patient's go home with a Band-Aid.
Am I a candidate for Ovarian Vein Embolization?
If you are experiencing any of the below symptoms you may be a candidate for embolization:
- Pelvic pain or aching around the pelvis and lower abdomen
- Bulging veins around the vulva, groin, leg, perineum or buttocks
- Swollen Vulva
- Dragging sensation or pain in the pelvis
- Feeling of fullness in the legs
- Low Back Pain
- Hemorrhoids
- Worsening of stress incontinence
- Worsening in the symptoms associated with irritable bowel syndrome
Pain is usually present for over 6 months, on one side but can affect both sides. The pain is worse on standing, lifting, when you are tired, during pregnancy and during or after sexual intercourse. The veins are also affected by the menstrual cycle/hormones and therefore the pain can increase during the time of menstruation. The pain usually is improved by lying down.
You don’t need to suffer. Accurate diagnostic tests and effective treatment options are available.
Appointments are available via an online video telehealth platform or in person at one of the offices in Los Angeles, Orange County or San Diego, depending on the doctor’s availability. Contact Us Today. Why should you choose us? Read here.
How is Pelvic Congestion Syndrome Diagnosed?
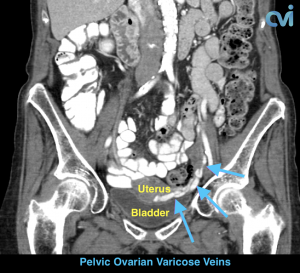
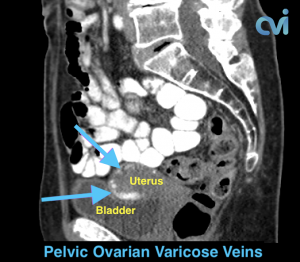
PCS can be diagnosed by Ultrasound or CT of the Abdomen and Pelvis.
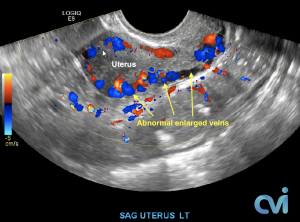
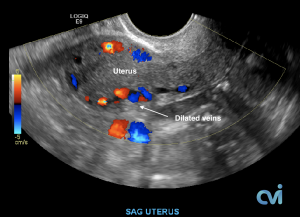
Ultrasound examination is the least invasive study and can identify enlarged veins around the uterus and pelvis. However, sometimes the veins in the pelvis are difficult to see or can be missed if the technician is not specifically looking in the right area.
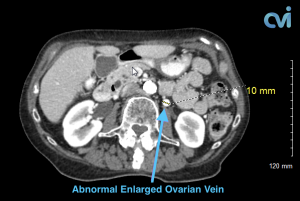
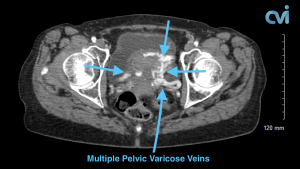
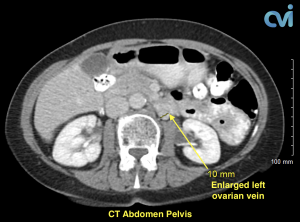
Magnetic resonance imaging (MRI) and computed tomography (CT) is another method to diagnose pelvic congestion syndrome. Our practice requires a CT of the Abdomen and Pelvis with contrast prior to treatment. This allows us to see where the varicose veins are coming from so that we can plan and do the appropriate treatment. Sometimes there are abnormal pelvic veins in addition to the ovarian veins that need treatment. Sometimes PCS can be missed on CT if the contrast injection is not timed appropriately or the vein is not directly measured.
Our specialist who is also a Board Certified Radiologist will review all of your imaging personally to make sure an accurate diagnosis is made. Following an accurate diagnosis, you can then undergo the Ovarian Vein Embolization procedure.
What are the Benefits of the Ovarian Vein Embolization?
- Outpatient, go home the same day
- Minimally Invasive, only requires a Band-Aid
- No stitches
- No major incisions
- No general anesthesia
- Proven safe and effective
- Least invasive
- Up to 80% of women have improvement in 2-4 weeks
Results
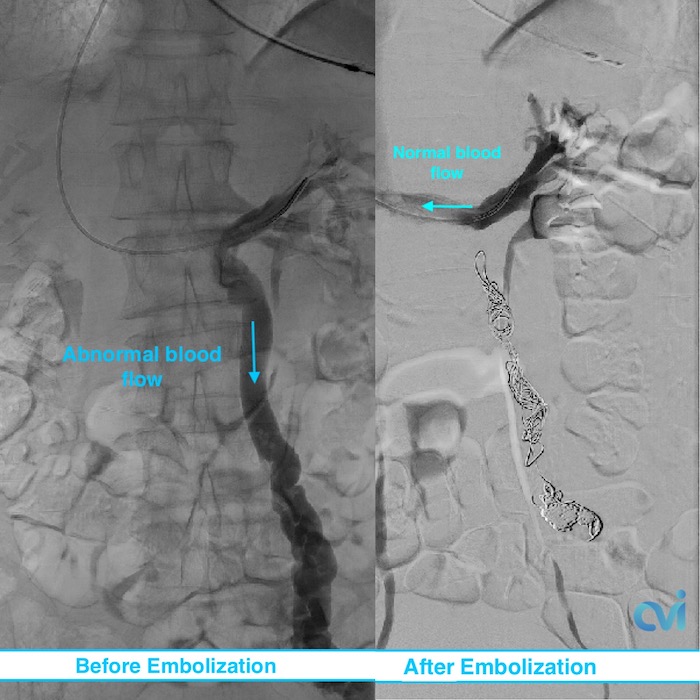
Embolization is a safe and effective treatment with minimal downtime and risk. Up to 80% of women report an improvement in symptoms within the first 2-4 weeks after embolization.
Appointments are available via an online video telehealth platform or in person at one of the offices in Los Angeles, Orange County or San Diego, depending on the doctor’s availability. Contact Us Today. Why should you choose us? Read here.
The above information explains what is involved and the possible risks. It is not meant to be a substitute for informed discussion between you and your doctor, but can act as a starting point for such a discussion.
